Salmonella
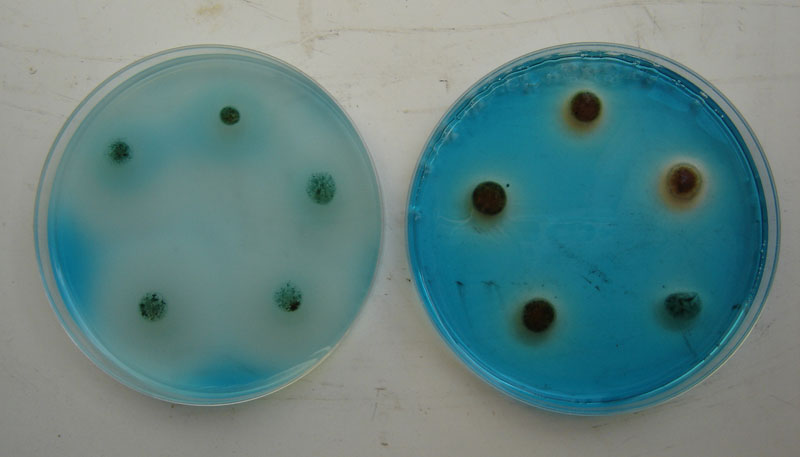
Salmonella MSRV - Positive and Negative
Salmonella
Bacteria belonging to the genus Salmonella are an important cause of food poisoning of humans. In certain parts of the world, Salmonella are also an important cause of disease in poultry. The genus consists of over 2,400 different ‘types’ called serovars. The serovars that are most relevant to the poultry industry are of the species known as Salmonella enterica. As an example, one of the more important serovars is S. enterica serovar Typhimurium. For the rest of this sheet, a brief terminology where the genus and serovar (but not the species name) is provided will be used, i.e., S. Typhimurium. Within some serovars, further sub-divisions – called phage types (PT) – are also recognised, e.g. S. TyphimuriumPT135.
Pullorum disease and fowl typhoid
Pullorum disease and fowl typhoid are septicaemic diseases that primarily affect chickens and turkeys, although other birds (quail, pheasants, ducks, peacocks and guinea fowl) are also susceptible. Pullorum disease (caused by S. Pullorum) was present in the commercial Australian poultry industry at a low level until the early 1970s but is now absent from the commercial industry. Fowl typhoid (caused by S. Gallinarum) has never been reported in Australia. Neither S. Pullorum or S. Gallinarum can infect humans and both are not found in any other Salmonella serovar – both serovars are non-motile.
Both pullorum disease and fowl typhoid remain a problem in Central America, South America, Africa and parts of Asia. In these parts of the world, the disease is a significant cause of economic loss.
Paratyphoid Salmonella
The motile Salmonella serovars associated with both animals and humans are commonly called paratyphoid Salmonella. These paratyphoid Salmonella are found in virtually all animals – both wild and domestic. In some animals, the infection is free of clinical disease and simply results in intestinal carriage, while clinical disease can occur in other animals.
In chickens less than seven days old, exposure to paratyphoid Salmonella with some serovars may result in intestinal colonisation and persistent, prolonged (though intermittent) shedding in the faeces. Depending upon the health of the chickens and the virulence of the particular Salmonella, there may be some mortality associated with invasion of these Salmonella outside the gastro-intestinal tract.
In mature chickens, clinical disease or mortality due to paratyphoid Salmonella is rarely seen. Depending upon the general health of the bird and the virulence of the particular strain, some paratyphoid Salmonella can move from the intestinal tract to internal organs. The most studied example is S. Enteritidis, which has been shown to be able to colonise the ovary and oviduct and can be deposited (albeit at a very low prevalence) inside eggs laid by infected hens.
Poultry, paratyphoid Salmonella and humans
Salmonellosis of humans caused by paratyphoid Salmonella is typically acute gastroenteritis following the consumption of contaminated food and is usually a self-limiting illness. A range of food products, including poultry, have been linked with human salmonellosis.
A range of paratyphoid Salmonella have been found in Australian chickens. However, not all of these poultry-associated Salmonella are capable of causing human disease. The most common paratyphoid Salmonella found in chickens is S. Sofia (36% of chicken isolates in one study and 90% in another study). However, S. Sofia is rarely isolated from ill humans. In addition, S. Enteritidis – the serovar that has caused major problems in the European and North American poultry industry – is rarely detected in Australian chickens.

Typical reaction of a Salmonella on one of the common identification media.
Management techniques
As many animals (rats, mice, wild birds) and insects (cockroaches, flies, beetles) can carry Salmonella, very good biosecurity is a necessity on the farm. Very active rodent control programs, strict restrictions of personnel and equipment movement and use of chlorinated water are all part of the standard management practices adopted by the Australian poultry industry. Routine checks for the presence of Salmonella are often undertaken. Within chicken meat processing plants, there are a number of steps taken (e.g. water chlorination, correct temperature controls) to ensure that contamination is prevented.
As Salmonella are heat sensitive, food-borne disease outbreaks are always associated with poor or inappropriate food hygiene practices. Effective cooking, good storage temperatures and practices that prevent cross-contamination (e.g. knives used to prepare raw meat should not be used to dice salad) will prevent food-borne illness. The Australian poultry industry maintains an active consumer education program to ensure that raw chicken meat is handled in a safe and appropriate manner, in the home and in the commercial food service industry.
The future
A range of innovative techniques, both at the farm level and in the processing plants, are currently being studied in Australia and elsewhere. As these techniques are validated and approved, they will be adopted by industry and will add to the ability of the industry to provide safe, healthy poultry products.

