Campylobacter
Campylobacter
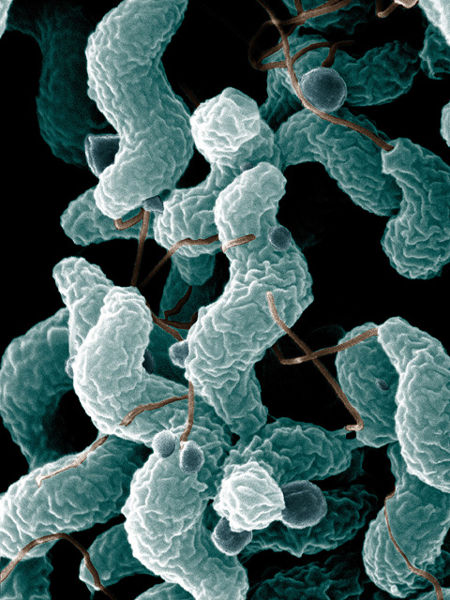
Campylobacter is the most common cause of infectious bacterial enteritis (food poisoning) worldwide. There are two species which cause human disease and Campylobacter jejuni accounts for over 90% of infections causing disease and Campylobacter coli making up the remainder. There has been increasing international concern at the rising incidence of Campylobacter infection worldwide.
Campylobacter infection displays marked seasonality, peaking in late spring and early summer. This may be due to changes in the shedding/colonisation of Campylobacter jejuni by the natural hosts and changes in human behaviour such as BBQs and swimming in non-disinfected waters, e.g. streams, which can lead to increased risk of exposure to Campylobacter. Both species of Campylobacter are found in the intestinal tract of a wide variety of wild or domesticated animals which show no sign of disease. In poultry, they multiply in the hindgut.
Symptoms of food poisoning
Campylobacter jejuni causes an illness known as Campylobacteriosis, which is more commonly known as gastroenteritis. The incubation period is two to seven days and infection in humans causes acute (bloody) diarrhoea lasting about five days, accompanied by fever and abdominal pain. The bacterial cells adhere to the walls of the intestinal tract where they damage the walls and produce toxins. The disease is usually self-limiting, however, approximately 0.05% of patients develop Guillain-Barre syndrome (a temporary inflammation of the nerves causing pain, weakness and paralysis) from which 25% recover, 1% suffer from reactive arthritis lasting from a few weeks to months, and 0.01% develop inflammatory bowel disease.
Sources of food poisoning
Campylobacter infections are considered to be mainly foodborne diseases in which foods of animal origin play an important role. Besides the food-related cases, close contact with pet animals and activities related to recreational waters contribute to a large number of human illnesses each year. Epidemiological studies have revealed an association of sporadic Campylobacter infection with consumption of undercooked chicken and dairy products as the primary foods associated with illness among older children (>5 years) and adults in Australia. Contact with puppies and pet chickens was also a significant risk factor. Large outbreaks of Campylobacteriosis are relatively rare, but implicated sources have been raw milk and untreated surface water. The majority of Campylobacter infections are sporadic single cases or small family outbreaks and the sources are rarely identified since often the suspected food has been consumed or is no longer available.
Farm level
The contamination of poultry originates in primary production. Studies have identified widespread animal and environmental sources of Campylobacter in the farming area, including:
- Domestic and farm animals including pet dogs and cats, wild birds, farm animals (cattle, sheep, pigs, ducks, turkeys)
- Insects (beetles, flies)
- Rodents (mice, rats)
- Environment – soil, air, water (swimming water, recreational streams, disinfected effluent, puddles, pond water, surface waters), protozoans, wild birds and wildlife
The key risk factor for introducing Campylobacter contamination into a poultry flock is human traffic into the shed. Other risk factors include equipment movements, staff working with cattle, growing broilers on mixed-species farms, flies, darkling beetles and their larvae, composting of dead broiler carcases, infection of the previous flock/inadequate cycle breaks between flocks, partial depopulation of a flock, puddles around sheds and surface water contamination. Possible intervention strategies for Campylobacter at farm level focus on address these issues as well as improved biosecurity and include:
- Hand washing/sanitising on entry to broiler shed
- Limiting access to broiler sheds to essential personnel
- Cleaning and disinfecting equipment moved between sheds e.g. scales
- No access of pets and livestock to the area surrounding the broiler sheds
- Hygiene barriers to be constructed in all sheds, where personnel step over the barrier and change to dedicated shed footwear
- Best practice guidelines for thinning of bird numbers in sheds to minimise risk
- Improved farm management practices – high levels of Campylobacter are more likely to be associated with flocks with poor litter management
- Sanitation of water supply
- Monospecific farms (no other farm animals)
- Improved cleaning and disinfection of sheds or extended breaks between flocks
- Improved darkling beetle/larvae control
However, it should be noted that intensified biosecurity, environmental and management programs have met with limited success in reducing the prevalence of flocks contaminated with Campylobacter.
Processing level
Additional measures in subsequent stages of the food chain may need to be developed to further reduce the contamination of poultry meat with Campylobacter. Methods such as rapid freezing, vacuum drying/cooling and chlorine sprays/chlorination of processing water are all methods currently being trialled worldwide.
Consumer level
Campylobacter-free poultry is not expected to be available in the short term. Cross-contamination in the kitchen has been identified as a major contributing cause of foodborne illness. Interventions to change consumer behaviour such as cleaning of kitchen utensils, cutting boards, taps etc. and rinsing of salads could significantly reduce the incidence of Campylobacteriosis.
Future action
International risk profiles and assessments for Campylobacter in chickens by bodies such as the World Health Organisation are underway with the overall objective to significantly reduce Campylobacter foodborne illness. Strategies for the reduction of Campylobacter in chickens will encompass primary production, processing and consumer education. Interventions aimed at reducing the contamination of poultry meat are expected to contribute significantly to a reduced incidence of illness in humans.

